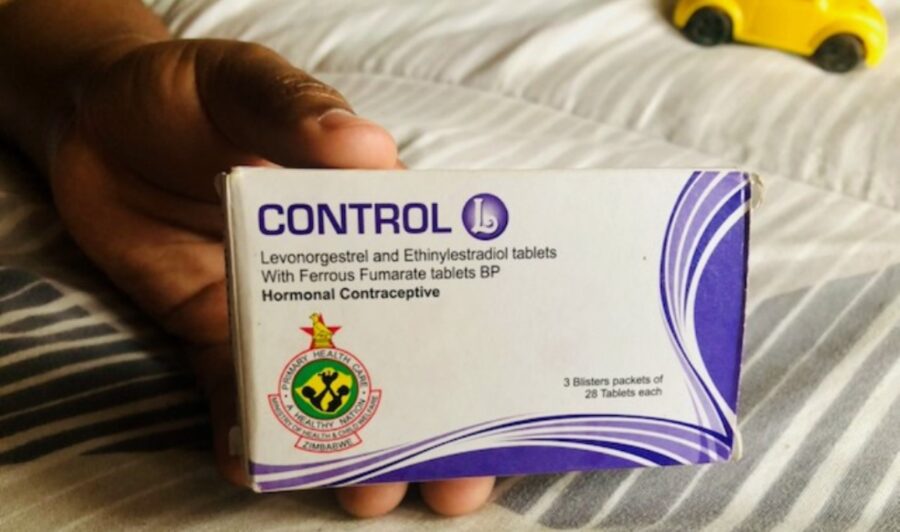
High Demand for Contraceptive Pills Smuggled in from Zimbabwe
With long queues at clinics in South Africa and Covid-19 restrictions, women struggling to access health services are turning to an illicit market for birth control pills. The pills are widely used and freely distributed in Zimbabwe, but smuggled into and sold in South Africa. Birth control pills freely distributed in Zimbabwe are being smuggled […]
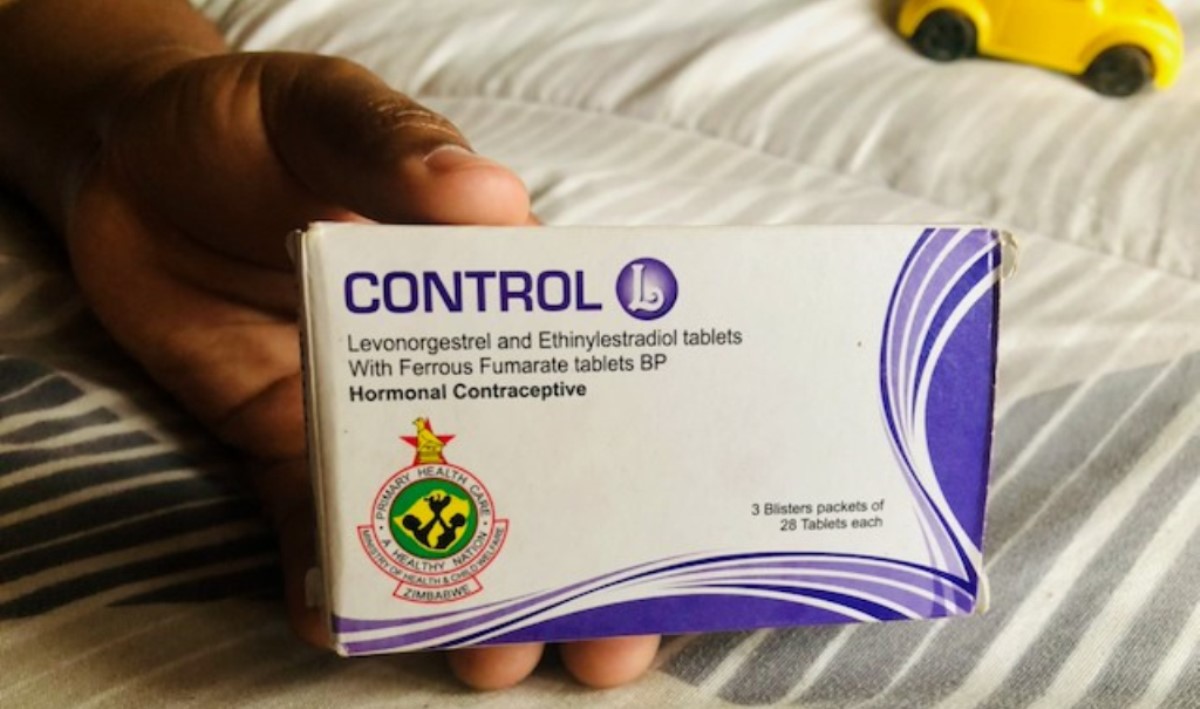
With long queues at clinics in South Africa and Covid-19 restrictions, women struggling to access health services are turning to an illicit market for birth control pills. The pills are widely used and freely distributed in Zimbabwe, but smuggled into and sold in South Africa.
- Birth control pills freely distributed in Zimbabwe are being smuggled into and sold in South Africa.
- Many Zimbabwean women prefer these pills above those from South African clinics.
- The market is fuelled by the struggle women have to access health facilities.
- Illicit marketeers say the trade is a godsend for them during Covid-19.
Familiar brands from back home are preferred by many immigrant Zimbabwean women instead of the brands supplied in South African clinics.
Smugglers of the pills say they also have demand from Mozambican, Malawian, Basotho and South African women.
GroundUp has previously reported on smuggling of contraceptive pills from Zimbabwe. The pills are supplied free by Zimbabwean clinics through the country’s Department of Health. But people who source the tablets for resale in South Africa get them in exchange for goods that are affordable in South Africa but expensive in Zimbabwe, or they pay clinic staff US$1 (R14.51) for a box of three blister packs of 28 tablets each. In South Africa they can sell each blister pack for R30 to R50, traders told GroundUp.
“I am expecting a batch of 500 pills, loaded safely on a bus from Zimbabwe as we speak,” a trader, who lives in Springs, told GroundUp. She also sells to sex workers and sometimes visits informal mining areas such as Payneville and Benoni, where people will pay R200 for a box of contraceptives.
She used to return to Harare and fetch stock sourced by her aunt back home. But Covid-19 travel restrictions have seen less opportunity for her to bring in the contraceptives herself. Cross-border trading, not only with contraceptives, has been her source of income for more than ten years.
“The long queues at clinics due to social distancing are proving to be a blessing in disguise. Women who used to queue at local clinics for family planning are buying from me now,” she said. “Especially during the toughest lockdown periods.”
“Some women say they would rather sacrifice buying bread to make sure they have money for contraceptive pills,” she said.
Another woman told GroundUp she sells directly from her door and takes orders through Whatsapp. She gets stock from her sister who “has connections in clinics” and lives in Chipinge. She says she runs out of stock because there is so much demand.
“Some suppliers ask for goods such as groceries, clothes and electric appliances such as TVs. I then buy the goods and send them in exchange for the pills. I sell the pill and make cash for myself,” she said.
“This is no longer about the brand of tablets but about convenience. At clinics women go through lots of processes to get contraceptives. They get tested for pregnancy first and one has to be on their period to get the pill or an injection. With us there are no such complications; we just sell them the pill,” she said.
However, a leading pharmacologist told GroundUp:
That is not entirely accurate – at the family planning or primary health-care clinics, when initiating hormonal contraception for the first time, the client would be asked about the last menstrual period, to exclude pregnancy. However, a negative pregnancy test is not an absolute requirement. This is what the guidelines state for the combined oral contraceptive (COC):
COCs may be initiated at any time, as long as it is reasonably certain that the client is not pregnant. If pregnancy cannot be ruled out (see Appendix 2: Pregnancy checklist), the client should be advised to avoid sex or use condoms until her next period starts, and start taking COCs on day 1 of her period (but not later than day 5). If her next period is late, she should come back for a pregnancy test.
He further advised:
The risks when women purchase hormonal contraceptives from unregulated sources include:
1. No screening for contraindications or adverse effects from prior use – these are prescription-only medicines for a reason
2. No screening for HIV and STIs
3. No consideration of other medicines which the women might be taking, and how those might interact with the contraceptive.
4. Being sold sub-standard or falsified products, or tablets which have not been stored appropriately and have deteriorated or expired (lost potency).Lastly, they are paying for something which should be available free of charge (though there are costs to accessing free care, in terms of transport or lost earnings).
If women who are undocumented migrants are either prevented from accessing services, or fear being refused or reported, that is also an issue that needs attention.
